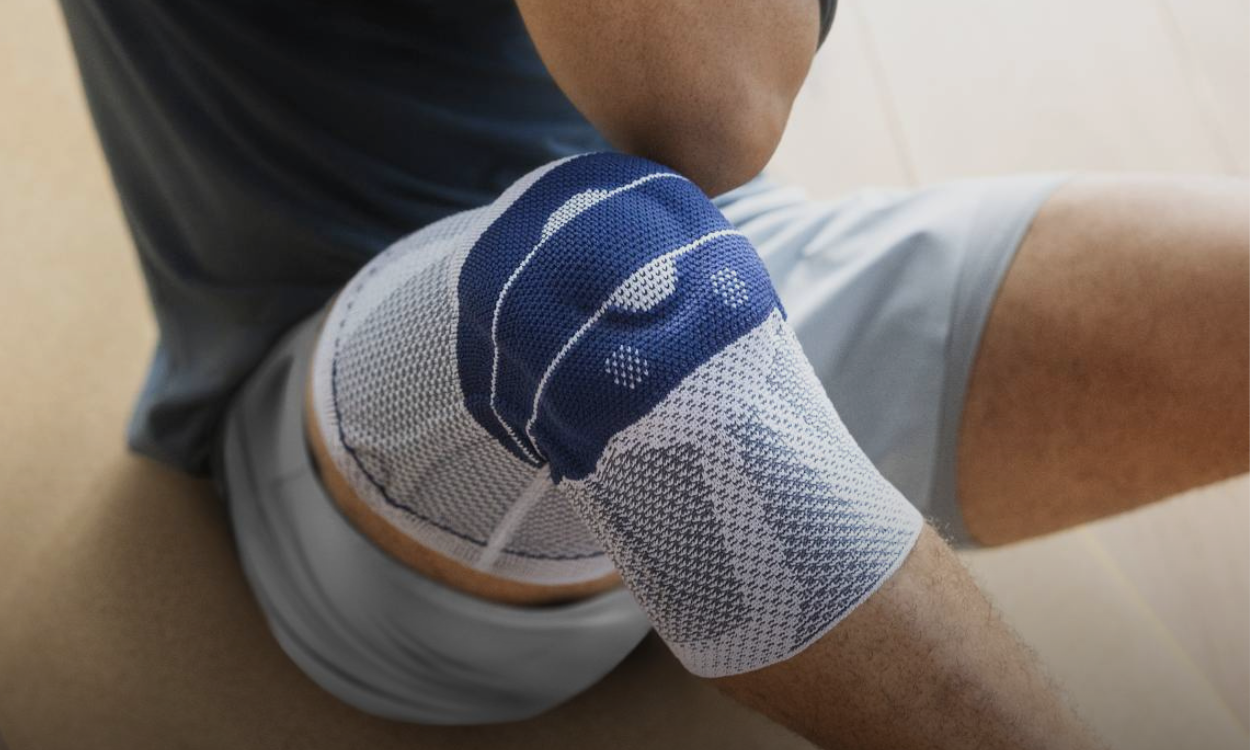
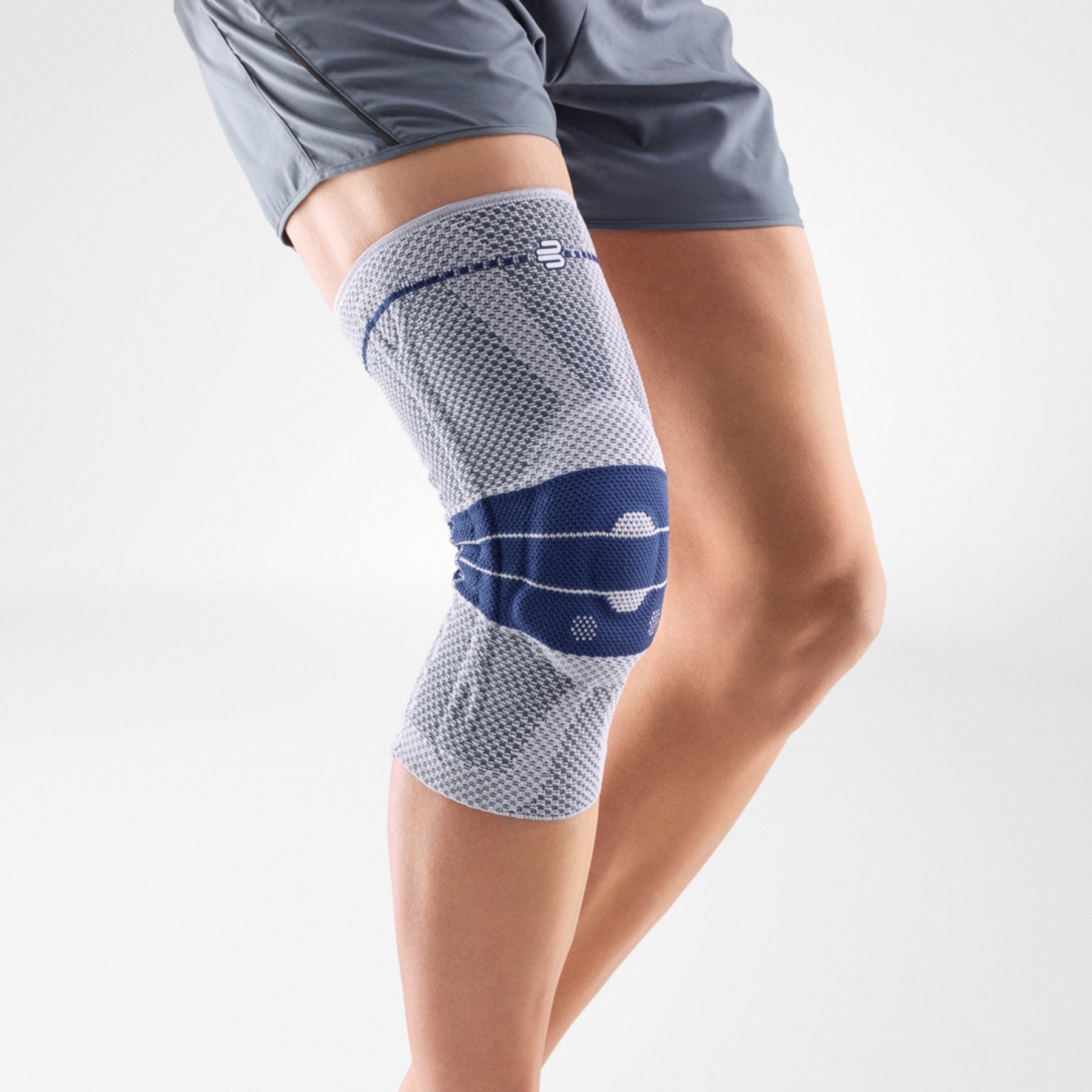
WHAT IS PHLEBOLYMPHEDEMA?
The circulatory system is responsible for transporting blood throughout our body and facilitates the transfer of oxygen from head to toe.
Our heart pumps the blood through our body, using a push and pull effect when it beats to allow for blood to travel back and forth effectively.


Phlebolymphedema is a disease where this excess fluid accumulates in the tissue around the blood vessels in the legs, ankles and feet.
A patient suffering from this condition experiences significant swelling in these areas.
Mild cases are managed conservatively if treated early, while chronic cases with long term neglect often result in restricted mobility and an overall drop in quality of life and would require more surgical treatment.
CAUSES OF PHLEBOLYMPHEDEMA
Phlebolymphedema is a disorder of the venous blood vessels in the lower legs. The veins aren’t strong enough to push blood against the pull of gravity. This results in pools of blood and fluid around the lower extremities of our body (legs, ankles and feet).
Some leading factors that lead to a Phlebedema include:
-
HEREDITARY/GENETIC PREDISPOSITIONS
-
LACK OF EXERCISE
-
OBESITY
PHLEBOLYMPHEDEMA SYMPTOMS
Phlebolymphedema (Phlebedema) is a progressive disease and the symptoms depend on what stage the condition is in. Some of the most commonly known symptoms include:
- Swelling in the legs due to long periods of inactivity (standing in one spot for a long time, sitting at a desk for extended hours)
- A heavy feeling in the legs, as well as fatigue when moving them.
- Tension on the skin around the legs, feet and ankles.
- Bulging of blood vessels and fluid within the legs. When pressed with a finger, these will slowly bulge out again.
- “Spider veins”, which are small excess veins that build up in the legs and prevent blood flowing effectively.

Long term wear and tear of the venous vessels may lead to chronic cases of Phlebolymphedema with serious complications including:
- Development of varicose veins (Twisted and enlarged veins).
- Increased risk of Thrombosis.
- Risk of developing mild ulcers and infections.
- Other related circulatory disorders.
An early diagnosis will lead to the most effective course of treatment when suspecting any of the mentioned symptoms.
DIAGNOSIS OF PHLEBOLYMPHEDEMA
A medical professional, in this case, a Phlebologist, begins with a complete physical examination to determine the progression of Phlebolymphedema.
Complete patient history is done to understand hereditary risks to the development of the venous drainage disorder.
Sophisticated imaging technology like the Doppler ultrasound scan can be used to detect the formation and location of blood pools in the lower half of the body. Early diagnosis results in the best prognosis and is highly recommended.
PHLEBOLYMPHEDEMA TREATMENT
Treatment for Phlebedema is mostly conservative. The condition is a direct result of a venous drainage disorder and results in pooled blood in our extremities. The condition progressively gets worse and early intervention is the most effective prognosis.
Treatment focuses on alleviating symptoms and managing the long term complications of the disease. A few proven measures include:
-
CHANGES IN LIFESTYLE
Simple changes in day to day lifestyle can have significant benefits in treating Lymphoedema. Regular exercise to lose weight and stay healthy reduces the stress on the arms and hands with swelling. Weight loss and reducing obesity often helps relieve pain and discomfort in most patients
-
REHABILITATION EXERCISE AND LYMPHATIC DRAINAGE MASSAGE
Targeted exercise can help manage weight as well as increase blood circulation through the affected arms and hands. Boosting blood circulation can help strengthen the muscles and facilitate healing.
Lymphatic drainage massage can also be used to stimulate the surrounding area and naturally encourage drainage of lymph fluid to alleviate symptoms.

-
COMPRESSION THERAPY
Compression therapy is the targeted application of pressure on the affected area using a medical compression garment. Compression garments like the VenoTrain Impuls can significantly improve a patient’s quality of life.
Regular use of a compression garment is instrumental in preventing the progression of Phlebedema, as the compression helps encourage the flow of lymph fluid out of the affected arm and can greatly reduce swelling and pain.
-
PRESCRIBED DRUG THERAPY
Anti-Inflammatory drugs can be used as prescribed by a medical practitioner. These can help in alleviating the accompanying symptoms and support the effects of compression therapy.
Everyday routine with a combination of the above helps slow and stop the progression of the disease and have immense long term benefits.
COMPRESSION GARMENTS FOR PHLEBOLYMPHEDEMA
Phlebologists highly recommend wearing compression stockings like the VenoTrain Micro on a regular basis.
This garment is an effective and instrumental tool in preventing the progression of the disease. In patients with the tendency of fluid build-up, the VenoTrain Micro provides graduated medical grade compression that encourages the natural drainage of fluids from the legs, helping not only to drain the fluid effectively but strengthen the circulation in the legs and pump blood up to the heart.

The breathable microfiber material (thinner than silk threads) exerts graduated pressure from the outside and helps strengthen the venous blood vessels and connective tissue in the legs, ankles and feet.
The VenoTrain Micro has been clinically proven to bring noticeable relief to patients suffering from Phlebedema whilst being comfortable for all-day wear.